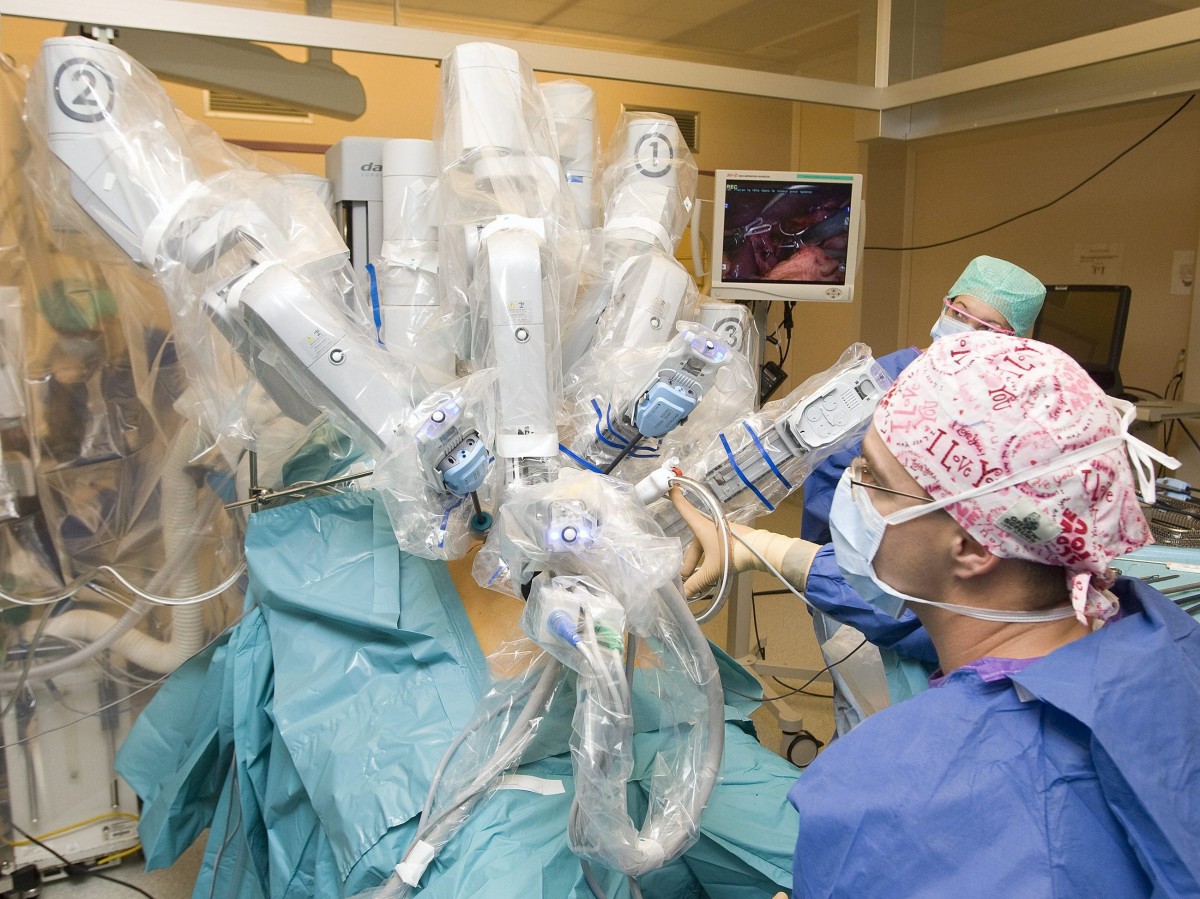
A recent study has found that problems encountered by medical professionals while using robotic surgical equipment, including deaths, were often reported late, inaccurately or not at all to the Food and Drug Administration.
The study, published in August in the Journal for Healthcare Quality, examined incidents over the last 12 years with Intuitive Surgical’s da Vinci Robotic Surgical System products.
Since surgical robots were first approved by the FDA in 2000, use of the equipment, specifically those designed by Intuitive Surgical, has increased dramatically, which is why the researchers said their findings were so concerning.
The FDA requires the information so that it can determine whether or not to approve a product. The agency also enters the information into its Manufacturer and User Facility Device Experience database. If a medical device malfunctions, hospitals are required to report the incident to the manufacturer, who in turn is supposed to report it to the FDA.
According to the study’s authors, only 245 incidents have been reported to the FDA in the past 12 years, which included 71 deaths and 174 nonfatal injuries.
In 2012, robotic surgery systems were used during about 367,000 procedures in the U.S. alone, an increase from 292,000 in 2011.
About eight in 10 of those procedures have been gynecologic or urologic procedures such as hysterectomies and prostatectomies, but other procedures that commonly use robotic equipment include coronary artery bypass, gallbladder removal, hip replacement, kidney removals and transplants, and cutting away cancer tissue from sensitive areas such as blood vessels, nerves or organs.
The researchers found that in at least five instances a report was never filed with the FDA. In three cases, one report wasn’t filed until 930 days after the surgery occurred, another was filed 292 days after the surgery, and the third was filed only after a media report told the story of a patient’s death.
While the study highlighted the benefits of using robots during surgical procedures, the researchers wrote that it is “essential that device related complications be uniformly captured, reported and evaluated” in order for the medical community to fully understand “the safety of the new technology.”
Martin Makary, an associate professor of surgery at the Johns Hopkins University School of Medicine, is a co-author of the study. Makary said that the findings are concerning since failure to report issues with the equipment means doctors are “not learning from our performance.”
However, the makers of da Vinci robotic equipment, Intuitive Surgical, took issue with the study and released a statement in September:
“The Journal for Healthcare Quality article gives the misleading impression that Intuitive Surgical has systematically failed in its obligation to timely report known adverse events to the FDA.
“Intuitive Surgical can only report adverse events after it becomes aware of them. We take this requirement very seriously and make every effort to account for all reportable events–even those from several years prior.”
Steven Schwaitzberg, an professor of surgery at Harvard Medical School, agreed. A two percent error rate is not bad, he said, but a new system should be implemented to track adverse events.
Makary added that given the number of those in the medical community who discuss using robotic technology, like the da Vinci products, the fact that only 245 adverse event (AE) reports have been filed with the FDA in a 12 year time period is suspicious. “We think that based on the sample, the 245 reported cases represent a small fraction of the true events out there,” he said.
Robotic surgery has been highly regarded by many in the medical field since it allows doctors to make smaller incisions, which result in shorter hospital stays for patients and less pain after their operation.
Between 2007 and 2011 the number of da Vinci medical robots used in the U.S. increased by 75 percent to 1,400 robots. According to a report from Medscape, as of June 2013, there were about 2,000 da Vinci systems installed in healthcare facilities throughout the United States.
However, a recent study of 16,000 women who had hysterectomies found that the robot operations didn’t reduce complications or blood loss, but raised a person’s risk of pneumonia post-surgery and cost about $2,000 more.
Who’s to blame when robotic surgery goes wrong?
During robot-assisted surgery, a surgeon sits at a nearby console that allows them to see a 3D view of the surgical site. Using the computer technology, the surgeon guides the robotic instruments inside the person’s body.
The technology has been applauded since if the surgeon’s hand trembles during surgery, the computer system is designed to ignore it. But the surgery doesn’t come without its risks, and in recent months leading experts in the medical field have begun to express concern about the safety and effectiveness of robotic surgery, especially because it is so expensive.
Since January at least 500 problems have been reported to the FDA regarding Intuitive Surgical’s robotic medical devices. One common issue reported is that the robot’s electrical currents “jump” from the robot into the patient’s body, which most often leads to serious injury.
As reported in the UK publication the Daily Mail, the electric charge can be prevented by putting protective plastic covers on the tips of the surgical instruments. But earlier this year the FDA reported that scraping the instruments against one another can lead to tears or holes in the plastic tips. The FDA said the manufacturer was not clear in its instructions to surgeons about this issue.
Even if there is no issue with the electrical currents, sometimes the procedures simply don’t go as planned. During an operation to remove a cancerous prostate gland, the camera attached to a robotic arm damaged one man’s bowels, which resulted in a severe infection, organ failure and cardiac arrest.
The man spent more than two months in intensive care and was later readmitted to the hospital with serious problems thought to be a result from the surgery mishap. Though the case sounds unique, it’s one of at least 26 lawsuits filed against Intuitive Surgical that involve complaints about punctured blood vessels or organs, severe bowel injuries or life-threatening infections such as sepsis.
One issue with robotic equipment is if something goes wrong during the procedure, who is to blame? The doctor, the hospital or the manufacturer?
Some say that any issues are a result of user error, such as a surgeon accidentally cutting through an artery because they can’t gauge its firmness. One way to fix that problem, according to experts at Johns Hopkins, is to better train surgeons on equipment before using it.
Currently, Intuitive Surgical requires a surgeon to do 20 surgeries under the supervision of another surgeon before they can perform them alone.
“If you as a patient are going to a doctor, and they’re using a robot, it’s a question of who’s in charge,” said James F. Blumstein, director of the Vanderbilt Health Policy Center and Professor of Constitutional Law and Health Law and Policy. “If it’s a mechanical malfunction, would the professional standard of care apply to a robot?
“If a doctor discloses to a patient there’s a comparative risk [between regular surgery and robotic surgery] and that disclosed risk materializes, I would have a hard time thinking the doctor would be considered negligent,” Blumstein added.
Though medical professionals are aware of these risks, Makary noted in the study that 37 percent of the U.S.-based hospitals that offer robotic surgery procedures neglected to mention any potential risks or complications on their website.
“We rely on a haphazard reporting system that uses immature data and only the best experiences make it into the data,” Makary said. “We introduce things but we don’t evaluate them very well. If we’re relying on the FDA about what [products] are superior, then we need a new process … you can’t make conclusions on the safety profile of a device based on a shoddy reporting system.”
In response, a spokeswoman for the FDA said that while the agency collects complaints and reports of adverse events, those alone are not enough for the agency to pull a product from the market. The agency also evaluates other information about a device’s safety and effectiveness, she said, but didn’t expand on what those other sources of information were.